|
Most of the selected studies were published from 2010 to 2019. The following combinations of keywords were used to initially select the articles to be evaluated: glioma and eloquent area glioma and tumor boundary glioma and function mapping glioma and infiltrative glioma and neuroplasticity. Literature review was electronically performed using the PubMed database. , With a deepened understanding of brain functional plasticity, staged surgery, or inducing functional plasticity preoperatively may represent a solution to this difficulty. Residual tumor will lead to recurrence or malignant transformation, affecting patient prognosis. The hindrance to the concept of “maximum safe resection” is residual tumor tissue in eloquent brain areas. ,, Tailored function mapping based on tumor location can permit more detailed functional assessments, which may further improve the functional prognosis of patients. Series of studies have been conducted on the mapping of higher-order cognitive functions such as calculation, attention, executive function, and memory. ,, In addition to technological innovation, the scope of functional protection is also expanding. nTMS both provide precise function mapping and play a unique role in the longitudinal study of functional plasticity. ,, Among the emerging brain mapping technologies, navigated transcranial magnetic stimulation (nTMS) has good applicability. ,, With direct cortical electrical stimulation, tumors in functional areas that were previously considered unresectable have been completely resected without neurological dysfunction. Among the available techniques, intraoperative direct electrical stimulation remains the gold standard for functional mapping. With the development of brain mapping technology, we can achieve individualized mapping of functional areas. The existence of individual differences and their impact on lesions make it impossible for us to rely on anatomical landmarks alone to protect eloquent brain areas. ,, , The current review will introduce some promising technologies at the experimental level, including the polarized light scattering imaging technique under development by our group. 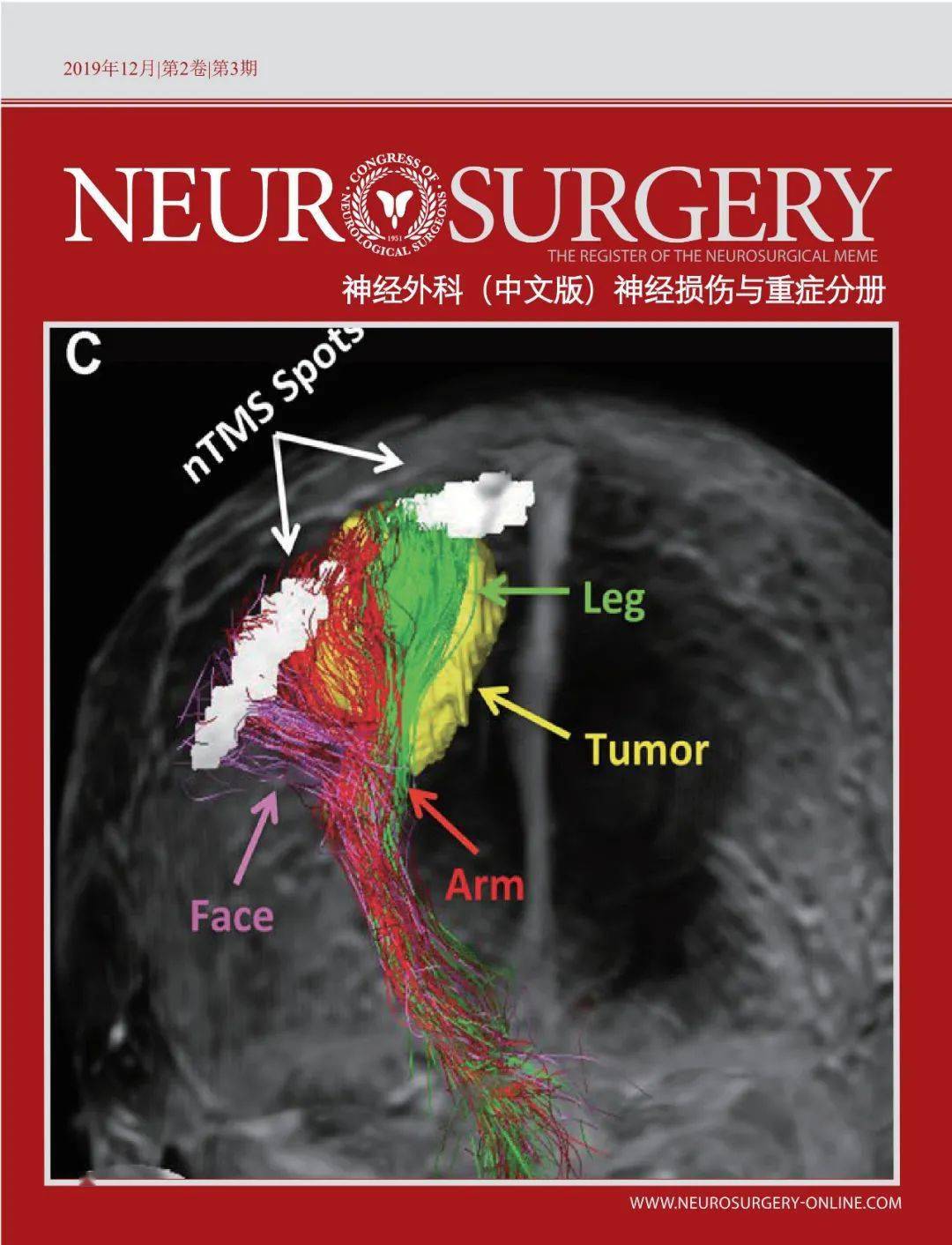
Preoperative multimodal imaging and intraoperative auxiliary technology can help improve the extent of glioma resection to radiological supratotal resection. , Experienced surgeons can judge the tumor boundary by sensing the change of brain tissue texture, color, and suction force, but it is difficult for even experienced surgeons to ensure a radiological total resection. Therefore, the balance between preserving neurological function and maximizing tumor resection has not been clarified.īecause of their infiltrative growth pattern, gliomas have no obvious boundary with brain tissue. The infiltration range of gliomas far exceeds the visible abnormal areas on routine images and often involves eloquent brain areas. ,, , However, gliomas often exhibit an infiltrative growth pattern, including extensive brain invasion. Several studies have revealed that the extent of surgical resection is closely related to patient prognosis. At present, the standard of care for glioma is comprehensive treatment based on surgical resection, which is the first and most important step of treatment. Gliomas are the most common primary tumors of the central nervous system. Surgical resection of glioma involving eloquent brain areas: Tumor boundary, functional boundary, and plasticity consideration. Keywords: Function mapping, glioma, neuroplasticity, surgical resection, tumor boundary This article reviews these three key points and highlights potential perspectives for the development of glioma surgery. The accurate identification of tumor boundaries, precise mapping of functional boundaries, and an in-depth understanding of functional plasticity are key factors for accomplishing this challenge. Thus, identifying the equilibrium between tumor resection and functional preservation remains a challenge in glioma surgery.  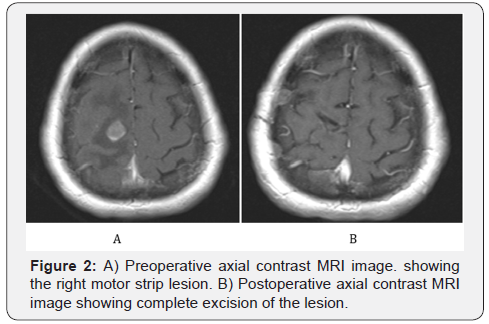
Glioma is the most refractory intracranial tumor, and its diffuse infiltrative growth characteristics make total resection impossible in a biological sense, especially when tumors invade eloquent brain areas.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
